Liberty Vision’s Y-90 Radiation System is not just for eye cancer
Imagine that there was an ophthalmic tool that could quickly treat a wide range of eye conditions by custom-tuning the treatment dose to achieve the effect you wanted.
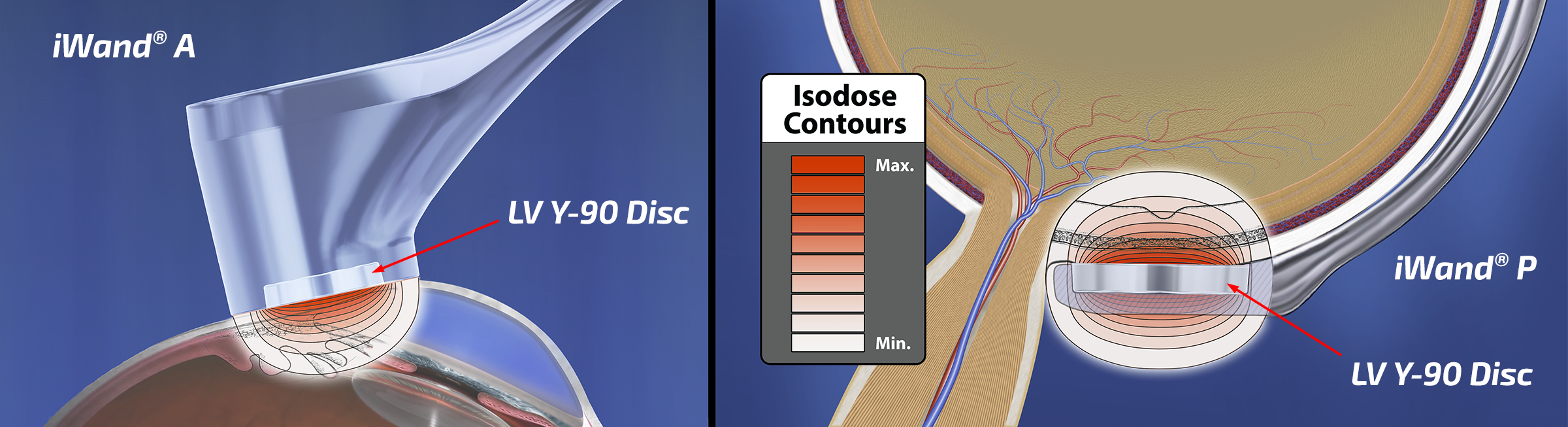
Liberty Vision has brought just such a tool to ophthalmic practice. It incorporates their disc-shaped, FDA 510(k) cleared, beta radiation disc mounted into one of their hand-held iWand® applicators for ophthalmic use.
In this article, we will describe how Liberty Vision’s variable strength and high dose rate (HDR) ophthalmic sources will change how tumors and benign ocular growths are treated on both the front and the back of the eye.
How Radiation Works and How to Take Advantage of Its Beneficial Effects
Radiation used for therapeutic purposes is called ionizing radiation because it forms ions (electrically charged particles) in the cells through which it passes.
For tumors, radiation distorts or damages the cellular DNA. During mitosis, the cancer cell’s DNA crumbles, leading to cancer cell death. These rapidly dividing cells are killed first, leading to tumor shrinkage, while normal cells divide relatively slowly or do not divide at all and thus stay functioning. Also, dependent upon the radiation source penetration depth, (from several millimeters to centimeters) resulting effects can take weeks or months to demonstrate a clinical effect.
Lower-dose radiation has been used to inhibit neovascularization, fibrovascularization, and inflammation in benign growths. Examples include pterygium, cutaneous keloid, or neovascular growths.
These conditions occur within millimeters of the eye wall (sclera). Therefore, radiation treatment at the surface or only millimeters deep is all that is needed, also limiting its effect on normal tissues.
The more precise the radiation, the less likely normal ocular structures will be affected. Radiation oncologists typically choose a particular radiation source and strength to achieve this goal in clinical practice.
How we can use beta-radiation to our advantage:
- Radiation affects vascular cell cytoplasm, which causes mechanical obstruction, leading to vessel thrombosis and closure. This effect is especially helpful for closure of unwanted neovascularization.
- New capillaries or vessels (neovascularization) are more rapidly growing and are thus more radiosensitive than established blood vessels. That way, the abnormal neovascular blood vessels are selectively closed.
- Vascular cells (endothelial and pericytes) in particular, are more radiosensitive than other mesenchymal cell types (skeletal or smooth muscle). Therefore, the abnormal blood vessels are affected rather than normal tissue.
- Radiation inhibits the inflammatory cell response, which is thought to play a role in choroidal neovascularization (CNV) and other eye diseases. For example, the decreased release of macrophage-mediated pro-angiogenic cytokines and growth factors, and vascular closures of abnormal blood vessels suppresses inflammation.
Therapeutic radiation was used to treat eye diseases such as retinal neovascularization since the early 1940s, and possibly earlier. However, prior techniques have suffered from mechanical or radiation delivery flaws, that limited clinical success. With Liberty Vision’s precise delivery and optimized engineering features, low-dose radiation can finally realize its huge potential for ophthalmology.
